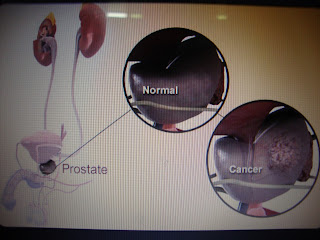
Age-Specific Reference Ranges for PSA in the Detection of Prostate Cancer
Age-Specific Reference Ranges for PSA in the Detection of Prostate Cancer
I am working in urology ward since 2001and used to sent PSA test for patient admission more than 50 years old,the urologist said,it is very important to get early information that patient have ca prostat from PSA report. many patient they don’t know about psa,from this articles we can get information about PSA test.
What is the prostate-specific antigen (PSA) test?
Prostate-specific antigen (PSA) is a protein produced by cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor takes a blood sample, and the amount of PSA is measured in a laboratory. Because PSA is produced by the body and can be used to detect disease, it is sometimes called a biological marker or a tumor marker.
It is normal for men to have a low level of PSA in their blood; however, prostate cancer or benign (not cancerous) conditions can increase a man’s PSA level. As men age, both benign prostate conditions and prostate cancer become more distinguish between benign prostate conditions and cancer. However, the doctor will take the result of the PSA test into account when deciding whether to check further for signs of prostate cancer common. The most frequent benign prostate conditions are prostatitis (imflamation of the prostate) and benign prostat hyperplasia or BPH (enlargement of the prostate). There is no evidence that prostatitis or BPH causes cancer, but it is possible for a man to have one or both of these conditions and to develop prostate cancer as well.
When is it ordered?
There is currently no consensus among the experts about when the PSA test should be ordered to screen asymtomatic males. Over-diagnosing, identifying cases of prostat cancer that may never cause significant health problems, must be balanced against missing the detection of aggressive cancers. There are national organizations, such as the National Cancer Institute and Centers for Disease Control and Prevention, that do not recommend routine screening at this time. Others, such as the American Cancer Society (ACS), recommend that doctors offer total PSA tests and DRE annually to all men, beginning at age 50 and to those at an increased risk of prostate cancer, such as American men of African descent and men with a family history of the disease, beginning at age 40 or 45. The ACS recommends that doctors discuss the testing options, benefits, and potential side effects with their male patients so that they can make informed choices. (See Prostate Cancer Screening for Adults and Adults 50 and Up.)The total PSA test and DRE may also be ordered when a man has symptoms that could be due to prostate cancer, such as difficult, painful, and/or frequent urination, back pain, and/or pelvic pain. Since these symptoms are seen with a variety of other conditions, including infection and prostatitis, the doctor will also frequently order other tests, such as a urine culture. Some of these conditions can themselves cause temporary increases in PSA levels. If a total PSA level is elevated, a doctor may order a repeat test a few weeks later to determine whether the PSA concentrations have returned to normal.
A free PSA is primarily ordered when a man has a moderately elevated total PSA. The results give the doctor additional information about whether the person is at an increased risk of having prostate cancer and help with the decision of whether to biopsy the prostate.
The total PSA may be ordered during treatment of men who have been diagnosed with prostate cancer to verify the effectiveness of treatment and at regular intervals after treatment to monitor for cancer recurrence. It is also ordered at regular intervals when a man with cancer is participating in “watchful waiting” and not currently treating his prostate cancer.
How the test is performed
Blood is typically drawn from a vein, usually from the inside of the elbow or the back of the hand. The site is cleaned with germ-killing medicine (antiseptic). The health care provider wraps an elastic band around the upper arm to apply pressure to the area and make the vein swell with blood.
Next, the health care provider gently inserts a needle into the vein. The blood collects into an airtight vial or tube attached to the needle. The elastic band is removed from your arm. Once the blood has been collected, the needle is removed, and the puncture site is covered to stop any bleeding.
reference range (PSA)
There has been recent guidance as to the level of PSA test that indicates further investigation is required (1). This reference range takes into account the patients age.
| AGE (YEARS) | PSA CUT OFF (ng/ml) |
| 50-59 | >=3.0 |
| 60-69 | >=4.0 |
| 70 and over | >5.0 |
PSA is also used as a means of monitoring disease:
Its main use is to monitor disease:
- if PSA > 40, there is a high chance that there is nodal or metastatic spread
- if PSA > 100, there is almost certainly metastatic spread
Reference:
- NHS Cancer screening programmes - Prostate Cancer Risk Management Programme (2002).